Tag Archive for: Peyronie’s Disease Treatments

Regenerative Medicine: Helping the Body Heal Itself
Medicine and science are seeing a promising new addition to their field where cells, tissues, and organs that had once been damaged are undergoing regeneration and repair, making them functional once more.
With regenerative medicine, the…

Transgender Hormone Replacement Therapy
It can be a distressing and confusing sensation when the physical features of your body do not match the gender you identify with. For those looking for a way to modify some of these features and feel greater peace with your body, transgender…

The Benefits of a Low Carbohydrate, High Fat Diet
With the many different diets bouncing around these days, it can be hard to tell which ones are worth following, and which ones will only cause more harm to your body despite their promise of fast results.
However, one diet linked to a significant…

The Effect of Nutrition on Essential Hormones
While we typically eat whatever foods seem the most appealing, the foods that we put into our body can significantly affect may aspects of our health, including hormonal balance.
Hormones are chemical messengers for the body and control…

The Relationship Between Autoimmune Disorders and Hormonal Deficiencies
Autoimmune diseases are becoming increasingly prevalent, especially among women. In fact, the American Autoimmune Related Diseases Association estimates that 80% of the 24 million Americans with autoimmune diseases are women, and 85% or more…
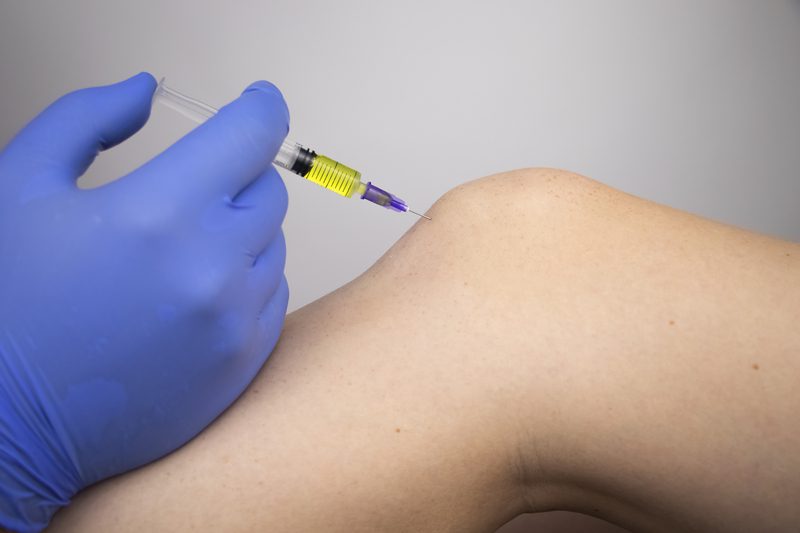
PRP Joint Injections
What Are PRP Joint Injections?
PRP joint injections involve the injection of platelet-rich plasma into an injured joint. This increases the concentration of growth factors at the injured site, accelerating the healing process.
The appeal…

The Benefits of Applying Progesterone to the Scrotum
Progesterone is very often considered for its role in pregnancy, and while it does play an important role in this process, it can also offer some benefits for men. Namely, progesterone cream may help how men feel and sleep while also maintaining…

IV Vitamin Therapy
What is IV Vitamin Therapy?
IV vitamin therapy provides a liquid mixture of vitamins and minerals through a small tube that is inserted into a vein. Whether you want to boost your immunity or enhance your beauty, the infusions are designed…
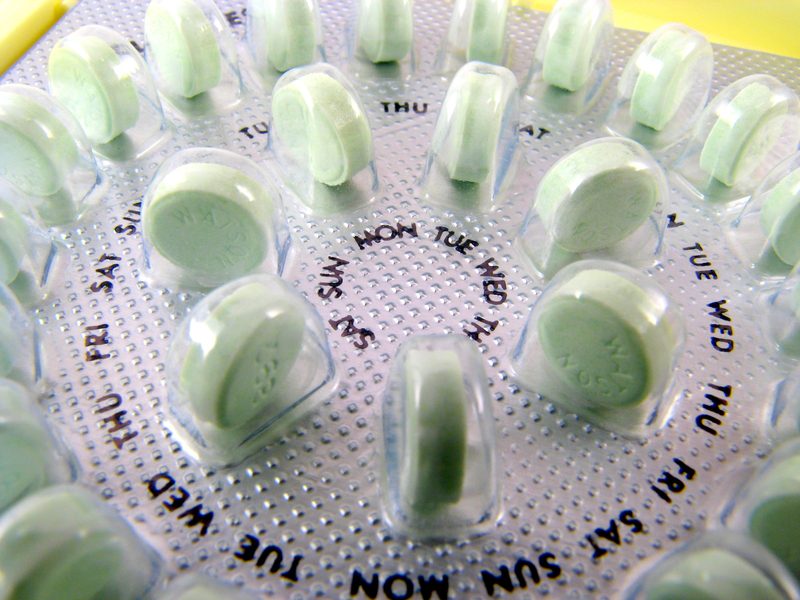
The Long-Term Effects of Hormonal Birth Control
When it comes to preventing pregnancy, hormonal birth control is one of the most popular options.
However, the uses of hormonal birth control often extend beyond just preventing pregnancy, with many women taking birth control to…

Dr. Melissa Irvine opens sexual health practice in Estero
Dr. Melissa Irvine opens sexual health practice in Estero
Offers treatments that improve quality of life for men and womenÂ
FORT MYERS, Fla. (April 5, 2022) – Dr. Melissa Irvine, DNP and Clinical Sexologist,…
